VISITING THE HMHC
Our permanent collections are operated by the Hennepin Health Foundation.
The collections are located in the lower level of the HCMC Blue Building – 915 S 8th St, Minneapolis, MN. MAP
Both collections are open:
Tuesdays and Thursdays
10am - 2pm and by appointment
The MMC Collection:
Is located in BL.227.
The HCMC Collection:
Is located in BL.226.
Email | 612.873.6090
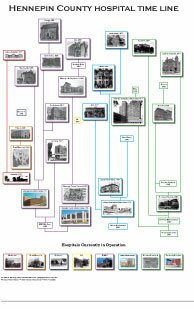
150 years of History
Enjoy a historical look of the hospitals from inception through mergers and transitions spaning 140 years. Read More
Partners
[partners]Welcome to the Hennepin Medical History Center!
The Hennepin Medical History Center at the Hennepin County Medical Center is a premier medical history museum celebrating the history of medicine and medical education in Minneapolis. The collection is like no other in the Twin Cities. The History Center is comprised of archives, rare books, artifacts and images of the history of the Hennepin County Medical Center and Metropolitan Medical Center, and their predecessors.
New Exhibitions!
The Hennepin Medical History Center is proud to announce a rotating exhibit featured in the Blue Lobby and Lower Level Blue Atrium walkway display cases. The exhibit, The World Within Our Walls, highlights the vast array of skills, abilities, and concerns that are necessary to fulfill our patient care mission. This exhibit contains historic and current documents, object, and photographs to tell the story of each hospital department’s contribution to our health care mission. These departments include; security, pharmacy, social service, spiritual care, facilities, business office, food service, storeroom and many more. The exhibit is developed and maintained by the volunteers and will assistance from the current staff members in the departments.
[links]Check out the new history blog! The website blog offers reflections and experiences by current and former HCMC employees and staff members about their work and careers at the Medical Center. The interviews were conducted and edited by Iric Nathanson and Thomas R. Mattison.
The current blog features Mary Croll.
HCMC History Collection
HCMC History Collection is a lively look at the field of health care, general patient care, and medical procedures at the Hennepin County Medical Center. Learn More
The Metropolitan Medical Center (MMC) History Collection
The Metropolitan Medical Center (MMC) History Collection, established in 1974, is dedicated to providing public access as well as preserving and collecting materials and artifacts that document the history of the MMC. Learn More
Educational History
There were many types of education programs at the hospitals in Minneapolis. Nursing schools were often unique to the specific hospital. Learn More